Psoriasis is a chronic inflammatory skin condition caused by rapid skin cell turnover, leading to thick, red, scaly plaques. It most commonly affects the scalp, elbows, knees, and lower back, but it can occur anywhere on the body. The disease results from an overactive immune response, where T-cells and dendritic cells trigger inflammatory cytokines that stimulate keratinocyte hyperproliferation, causing skin cells to accumulate on the surface.
Psoriasis
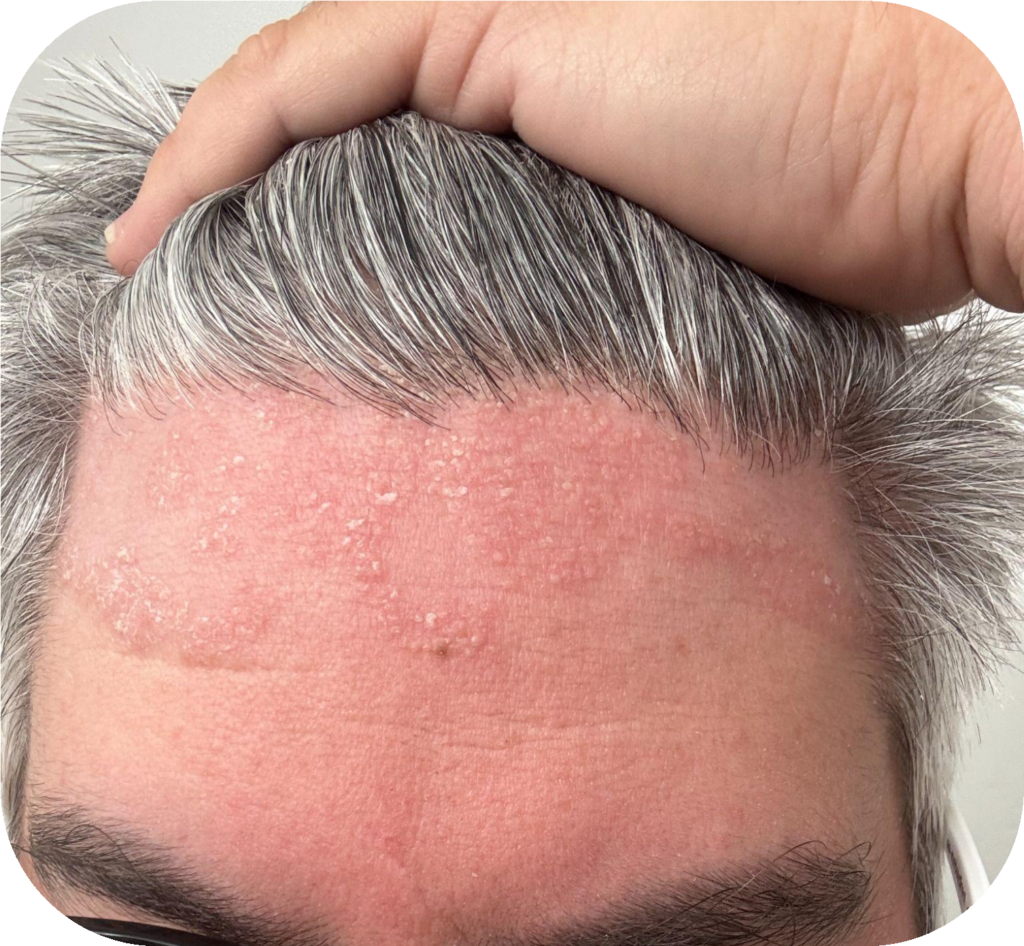
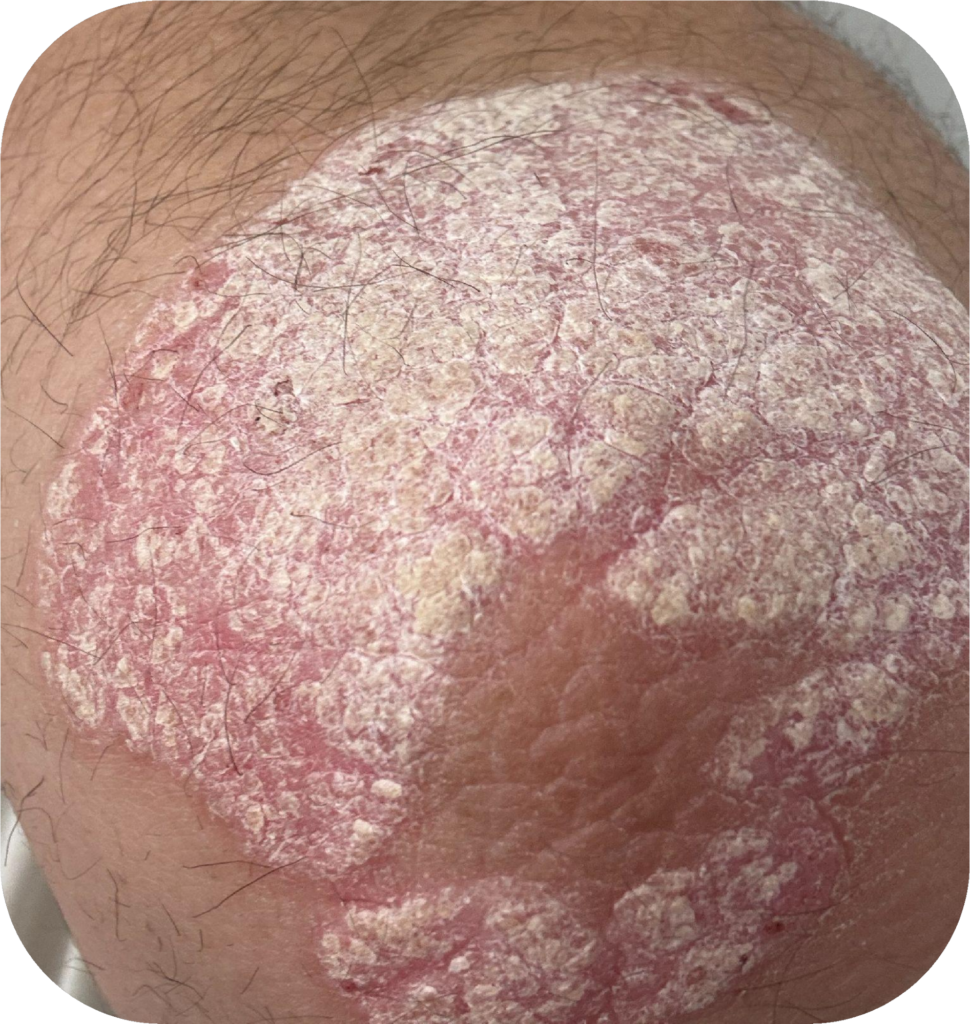
Psoriasis
Psoriasis is not just a skin disease, it is a systemic inflammatory condition that may also involve the nails and joints and is associated with psoriatic arthritis, cardiovascular disease, obesity, and metabolic syndrome. Because of these broader health connections, proper diagnosis and management are important for both skin improvement and overall health.
Common Variants of Psoriasis Psoriasis can present in several clinical forms:
- Plaque Psoriasis (Psoriasis Vulgaris): Most common type with well-defined red plaques and silvery scale.
- Guttate Psoriasis: Small, drop-shaped lesions that often appear after infections such as strep throat.
- Inverse (Flexural) Psoriasis: Smooth red inflammation in skin folds such as the groin, underarms, and beneath the breasts.
- Sebopsoriasis: Overlaps with seborrheic dermatitis and commonly affects the scalp, eyebrows, and sides of the nose.
- Pustular Psoriasis: Characterized by sterile pustules on inflamed skin.
- Erythrodermic Psoriasis: Rare but severe form with widespread redness and scaling.
- Nail Psoriasis: Causes pitting, thickening, discoloration, or nail separation.
- Psoriatic Arthritis (PsA): Inflammatory arthritis associated with psoriasis that causes joint pain, stiffness, and swelling.
Recognizing these variants helps guide accurate diagnosis and appropriate treatment, as different forms may require different management approaches.
Lifestyle & Metabolic Health
Chronic skin conditions such as psoriasis and eczema are closely linked to overall health. Factors including weight, diet, vitamin levels, inflammation, and blood sugar can influence how often skin flares occur. Treatment focuses on reducing inflammation, slowing skin cell growth, and relieving symptoms such as redness, scaling, and itching, while lifestyle changes can help improve long-term skin control.
Maintaining a healthy weight can reduce inflammation and improve skin symptoms. Helpful habits include an anti-inflammatory diet with lean proteins, healthy fats, low-glycemic carbohydrates, and fiber from vegetables, fruits, and whole grains. Regular exercise, such as 30–45 minutes of walking or cycling most days, along with strength training, is also beneficial. Some patients may also benefit from time-restricted eating (an 8–12 hour eating window).
Good liver health supports metabolism and inflammation control. Ideally, ALT levels should remain below 40 U/L. This can be supported by avoiding alcohol, staying well hydrated, and maintaining regular meal timing. Vitamin D supports immune balance and skin health. Ideal levels are 50–70 ng/mL. Many patients benefit from Vitamin D3 (about 5000 IU daily) with Vitamin K2, along with safe sun exposure.


Inflammatory skin diseases are linked to higher cardiovascular risk, so maintaining healthy cholesterol and blood pressure is important. Ideal targets include LDL <100, HDL >40, and blood pressure <120/80. A nutrient-dense diet, fiber, omega-3 fatty acids, magnesium, stress reduction, and limiting salt can support heart health. Reducing overall inflammation may also improve skin symptoms. Ideally hsCRP should be below 1.0 mg/L. Helpful habits include eating colorful fruits and vegetables, anti-inflammatory foods like turmeric and green tea, along with good sleep, regular exercise, and stress management.
Balanced blood sugar is also important. The goal is A1C below 5.7%, supported by a low-glycemic, high-fiber diet and regular exercise. Some patients may also benefit from supplements such as berberine or magnesium. Supporting immune balance can help reduce inflammation. Helpful nutrients include Vitamin D, omega-3 fatty acids, probiotics, curcumin, and Vitamin A, while limiting refined sugars, processed foods, and excess carbohydrates.
Psoriasis




Medical Treatments
Topical Treatments (Mild to Moderate Psoriasis)
Many patients begin treatment with medications applied directly to the skin. Topical corticosteroids are commonly used to reduce redness, swelling, and itching. They are effective but long-term use may cause skin thinning or stretch marks, so they must be used carefully.
Vitamin D creams, such as calcipotriol, help slow the growth of skin cells and reduce inflammation. Mild skin irritation can sometimes occur.
Topical retinoids, such as tazarotene, help normalize skin cell growth but may cause irritation and should not be used during pregnancy.
Calcineurin inhibitors (tacrolimus and pimecrolimus) help calm immune activity in the skin and are especially useful for sensitive areas such as the face, eyelids, or skin folds.
Tapinarof is a newer topical medication that helps regulate inflammation and improve the skin barrier. Some patients may experience mild irritation or folliculitis.
Other supportive treatments such as coal tar, salicylic acid, and moisturizers can help reduce scaling and soothe irritated skin.
Oral Medications (Moderate to Severe Psoriasis)
For more severe or widespread psoriasis, oral medications may be used.
Methotrexate helps reduce inflammation and slow skin cell growth but requires monitoring because it can affect the liver and blood cells.
Cyclosporine suppresses the immune system and can work quickly, but long-term use may lead to high blood pressure or kidney problems.
Acitretin is a vitamin A–based medication that helps normalize skin cell growth. It may cause dryness, elevated cholesterol, and serious birth defects if taken during pregnancy.
Light Therapy (Phototherapy)
Phototherapy uses controlled ultraviolet (UV) light to reduce inflammation in the skin and slow skin cell growth. It is often recommended for moderate psoriasis or when topical treatments are not enough.
Narrowband UVB is the most commonly used and safest form of phototherapy.
PUVA therapy combines a light-sensitizing medication with UVA light.
While effective, it carries higher risks such as skin aging, burns, and increased skin cancer risk with long-term use.
Tanning beds are not recommended for psoriasis treatment because they increase the risk of skin cancer and skin damage.
Biologic Treatments for Psoriasis
Biologic medications are advanced treatments used for moderate to severe psoriasis. They work by targeting specific parts of the immune system that cause inflammation and rapid skin cell growth, helping to improve plaques, redness, and scaling.
Several types of biologic medications are available. TNF inhibitors, such as adalimumab (Humira) and etanercept (Enbrel), reduce inflammation by blocking TNF-α. These medications can be effective but may increase the risk of infections, including possible tuberculosis reactivation, so monitoring is required.
IL-12/23 inhibitors, such as ustekinumab (Stelara), block immune signals involved in psoriasis. They are usually given by injection every few months and are generally well tolerated.


For people with moderate to severe psoriasis or psoriatic arthritis, biologic treatments can significantly improve symptoms and quality of life when used under medical supervision.
IL-17 inhibitors, including secukinumab (Cosentyx) and ixekizumab (Taltz), target a key inflammatory pathway in psoriasis and often provide rapid symptom improvement. Possible side effects include yeast infections and occasional worsening of inflammatory bowel disease.
IL-23 inhibitors, such as guselkumab (Tremfya) and risankizumab (Skyrizi), target another important immune signal that drives psoriasis. These newer medications often provide long-lasting control and are typically given every 8–12 weeks after the first doses.
Most biologics are given as injections under the skin, with dosing ranging from weekly to every few months. Because they affect the immune system, patients need screening and monitoring for infections.
Personalized Psoriasis Care
Psoriasis treatment works best when it is personalized for each patient. Many people benefit from a combination of lifestyle improvements and medical treatments to control inflammation and reduce flare-ups. At Aesthetics and Medical Lasers of Colorado, we provide comprehensive evaluation and customized treatment plans to help patients manage psoriasis and improve overall skin health.
Locations
Longmont: 700 Tenacity Drive, #102, Longmont, CO 80504
2801 Remington Street Suite 2, Fort. Collins, Colorado, 80525
Contact
720-818-0533
Office Hours
Monday-Friday 8:00 AM to 6:00 PM Saturday 10 AM to 2 PM Sunday: By Appoinment only

Aesthetics & Medical Lasers Dermatology
Get a Dermatology consultation and customized skin care solutions
Services
Work Hours
- Monday-Friday 8:00 AM to 6:00 PM Saturday 10 AM to 2 PM Sunday: By Appoinment only
- 720-818-0533
- 700 Tenacity Drive #102 Longmont, Colorado, 80504
- 2801 Remington Street Suite 2, Fort. Collins, Colorado, 80525
- Copyrigt © 2026 Aesthetics & Medical Lasers Dermatology
- Terms of Use
- Privacy Policy
