Allergic Contact Dermatitis (ACD) is a type of eczema that happens when your skin reacts to something it has become sensitive
Allergic Contact Dermatitis
Introduction to Allergic Contact Dermatitis
Allergic Contact Dermatitis (ACD) is a type of dermatitis (eczema) that happens when your skin reacts to something it has become sensitive to. Unlike irritant dermatitis (which comes from direct skin damage), ACD is an immune reaction—specifically a delayed (Type IV) hypersensitivity response. This means the rash usually shows up 24–72 hours after contact with the trigger.
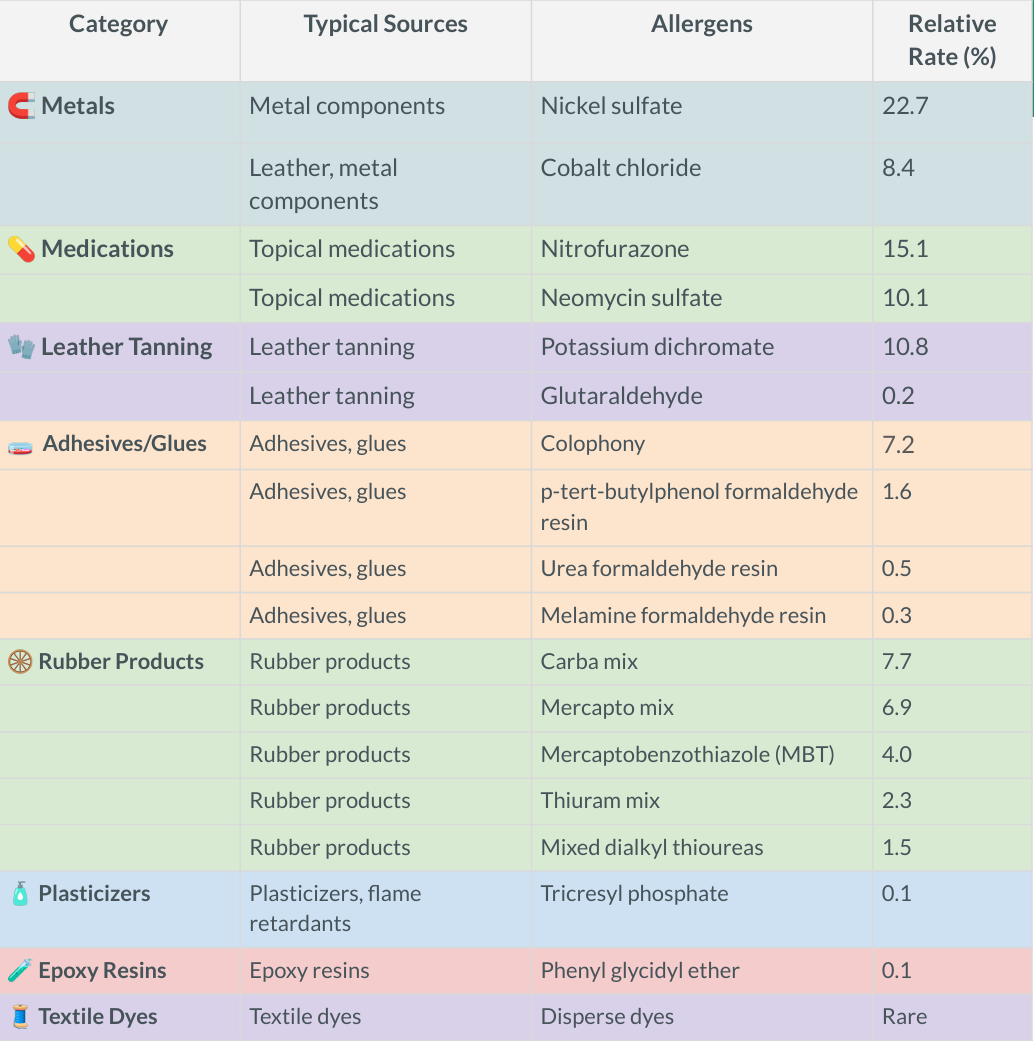
Common causes include fragrances, preservatives, nickel and other metals, rubber, dyes, certain plants (like poison ivy), and ingredients in skincare or personal care products.
Causes and Pathophysiology
ACD develops after your body becomes “sensitized” to a substance. When you’re exposed again, your immune system (T-cells) triggers inflammation, leading to redness, itching, swelling, and sometimes blistering or scaling. It can happen to anyone, but repeated exposure and a weakened skin barrier increase the risk.
Key takeaway
Once your body becomes sensitive to a trigger, it can react every time you’re exposed—so avoiding the allergen is the most important step in preventing flare-ups.
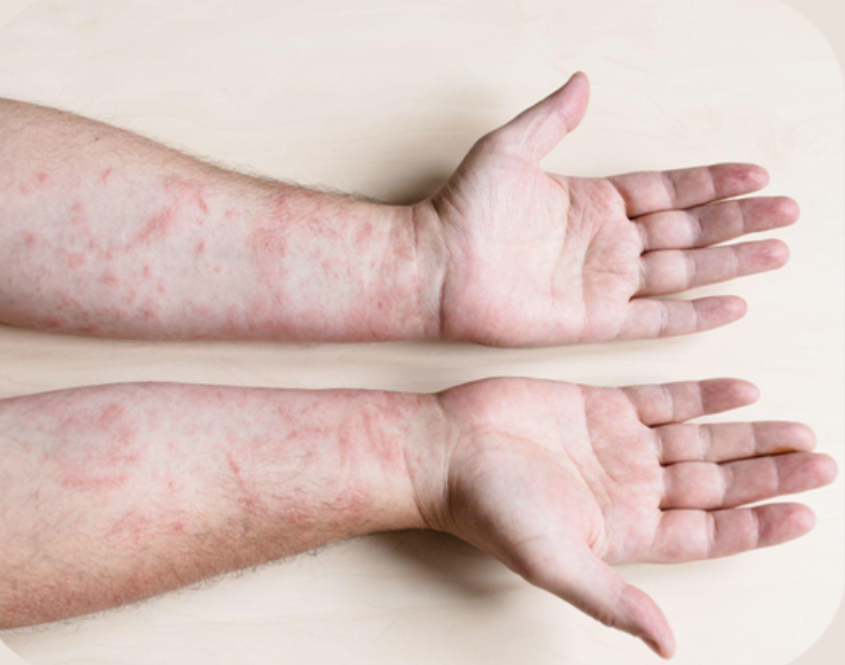
Allergic

Patch Testing
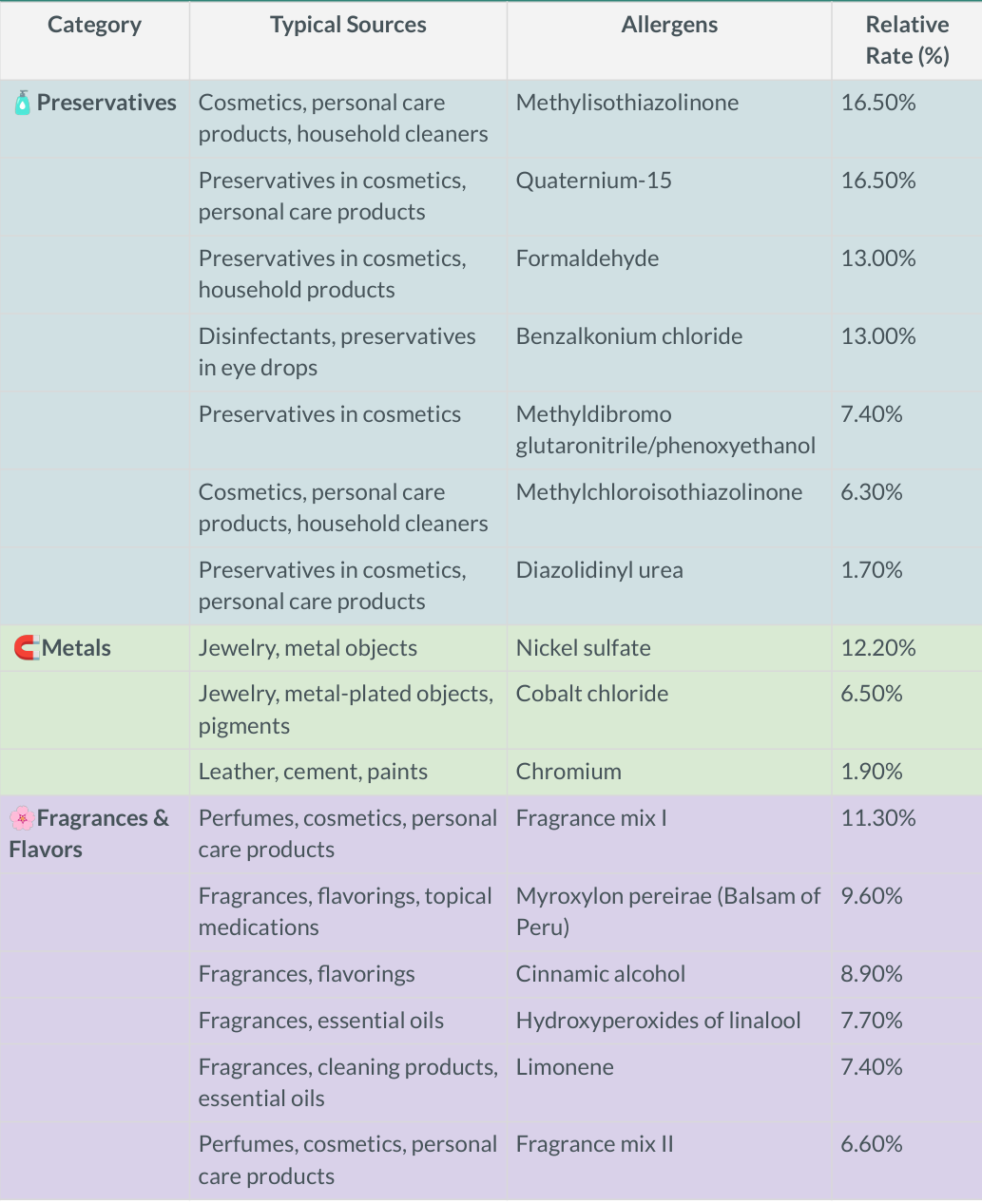
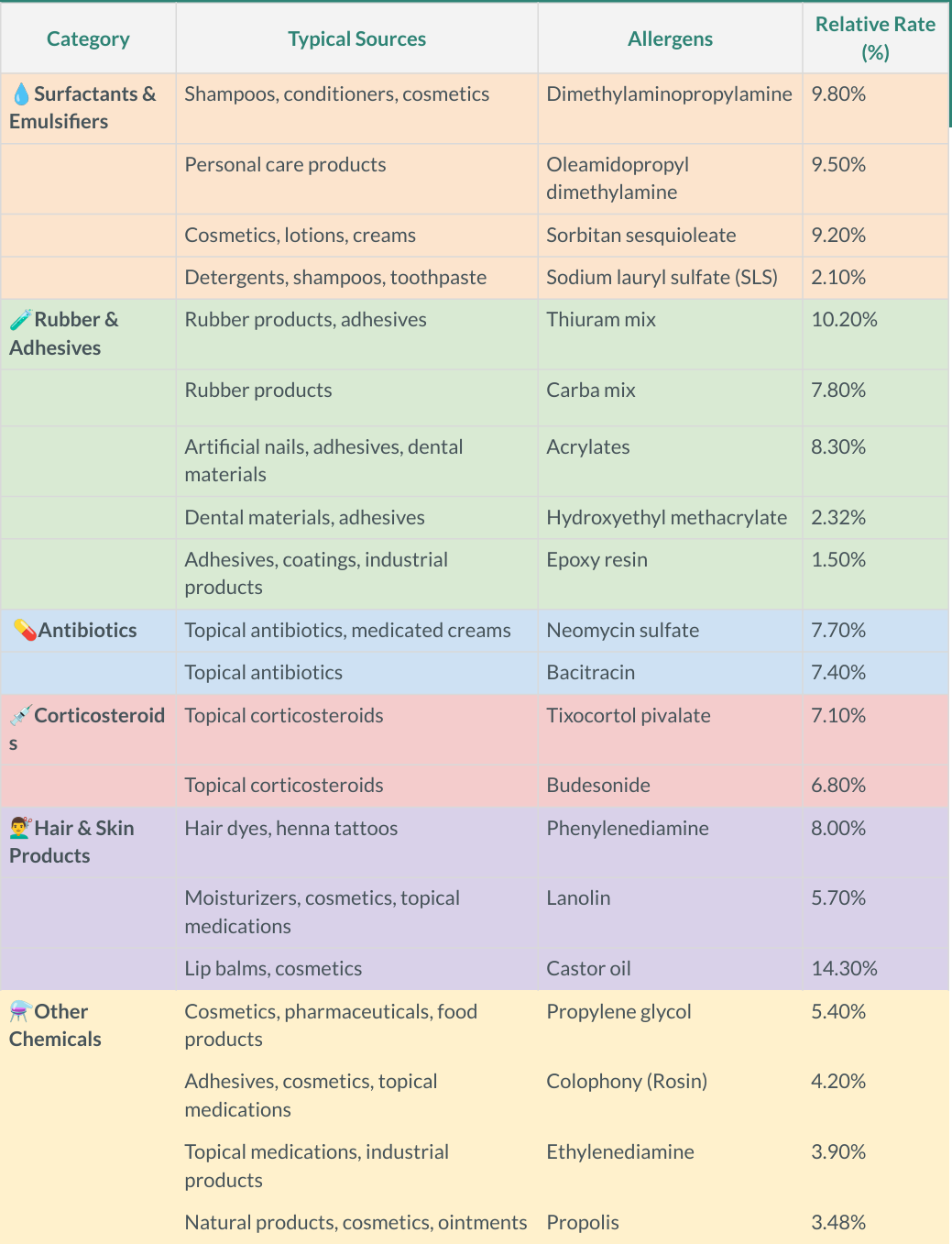
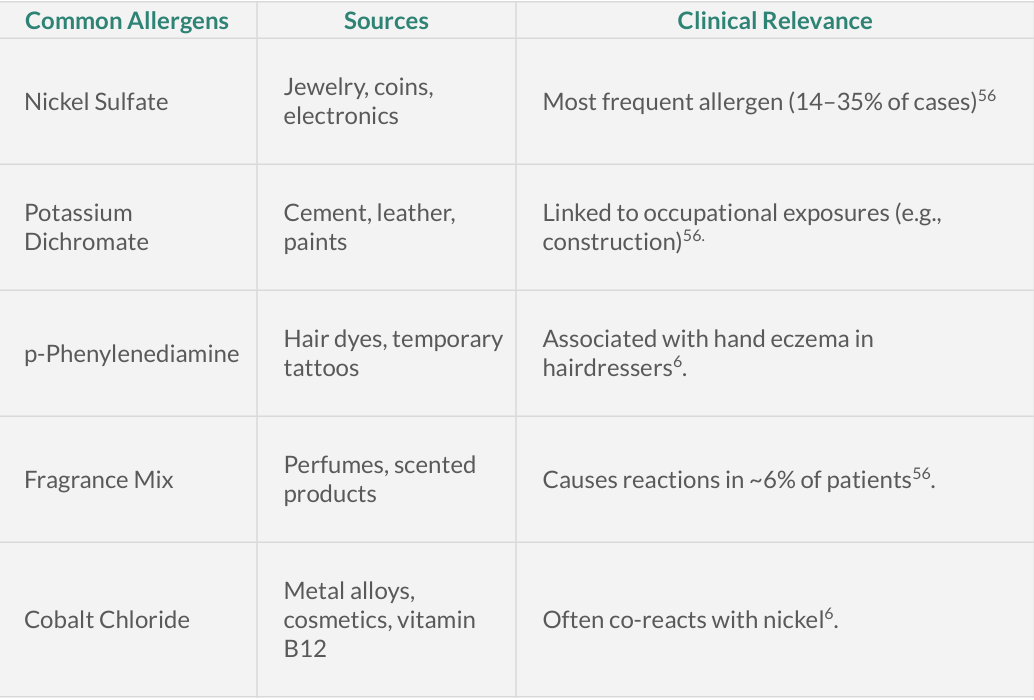
Patch testing is a simple, in-office diagnostic test used to identify the specific substances causing allergic contact dermatitis. Small amounts of common allergens (such as fragrances, metals like nickel, preservatives, and chemicals) are applied to the skin—usually on the back—using adhesive patches.
These patches remain in place for about 48 hours, and the skin is then checked over several days for delayed reactions. If a reaction occurs, it helps pinpoint the exact trigger. Patch testing is especially useful for patients with persistent or unexplained rashes, as it allows for targeted allergen avoidance and more effective long-term management.

Hand Dermatitis Causes
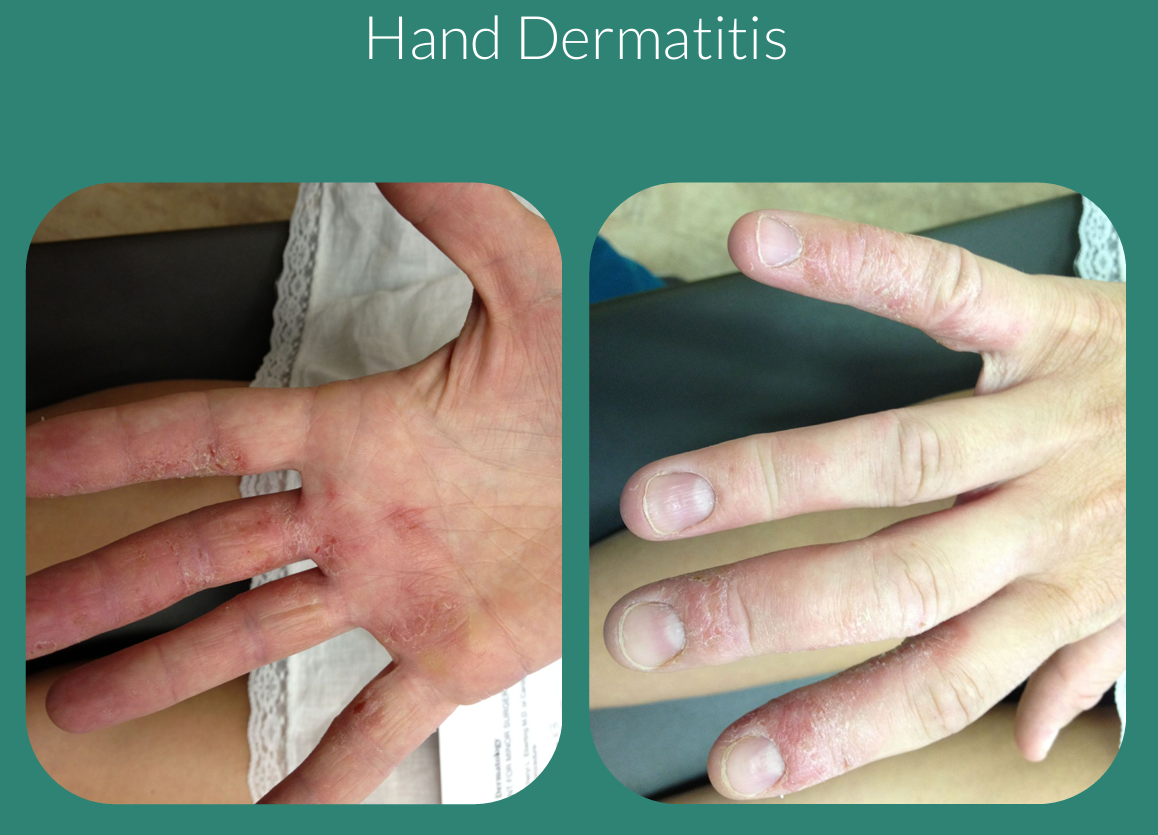
Pompholyx (Dyshidrotic Eczema)
Pompholyx, also called dyshidrotic eczema, is a type of eczema that causes small, intensely itchy blisters on the hands and feet—especially on the sides of the fingers, palms, and soles.

What it looks like
- Tiny, deep-seated blisters (often described as “tapioca-like”)
- Severe itching or burning
- Peeling, dryness, and cracking as it heals
Common triggers
- Stress
- Sweating or heat
- Allergens (like nickel or fragrances)
- Irritants (soaps, detergents, hand sanitizers)
- Sometimes associated with atopic dermatitis or contact dermatitis
Key takeaway
Pompholyx often comes and goes in flare-ups and can be linked to both irritants and allergic contact dermatitis, so identifying triggers (sometimes with patch testing) is important for long-term control.
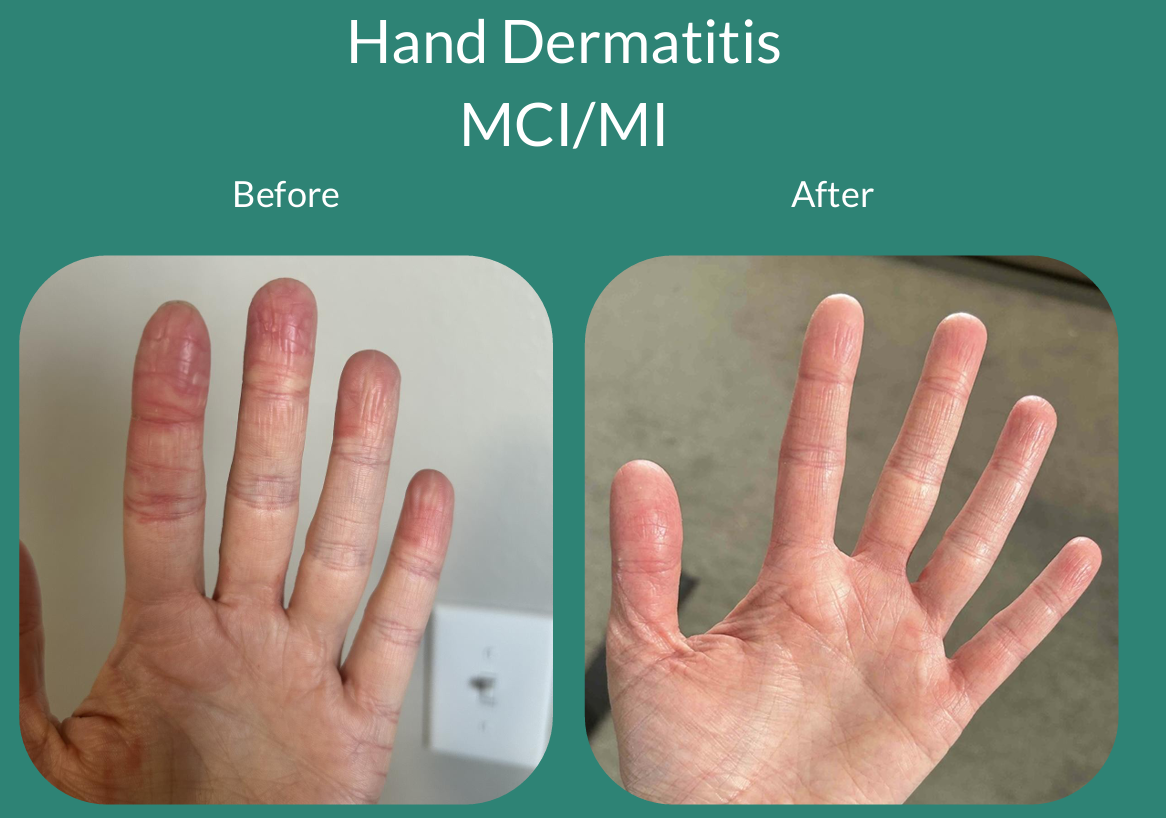
Hand Dermatitis MCI/MI

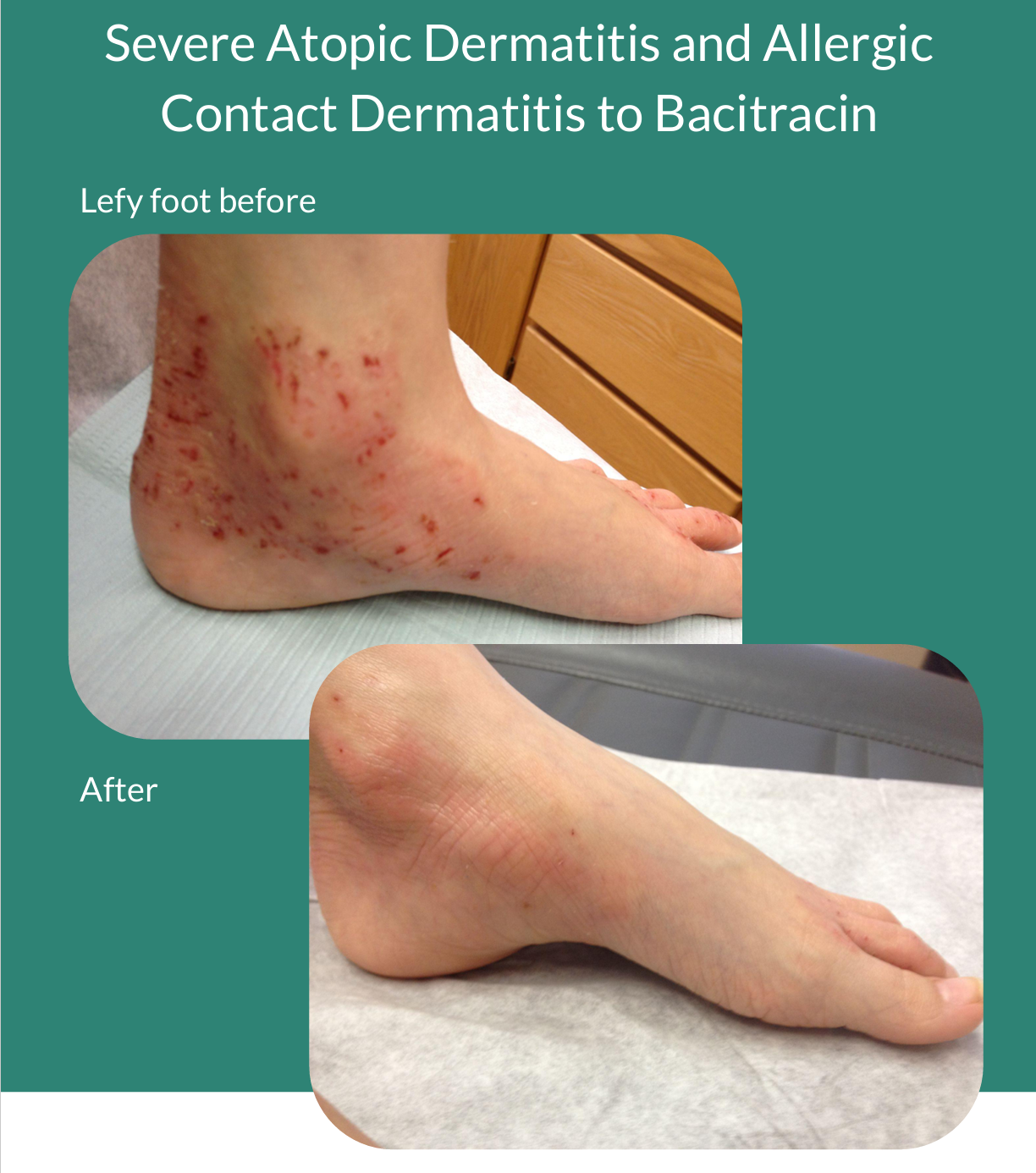
SHOE / FOOT DERMATITIS
Lip Dermatitis
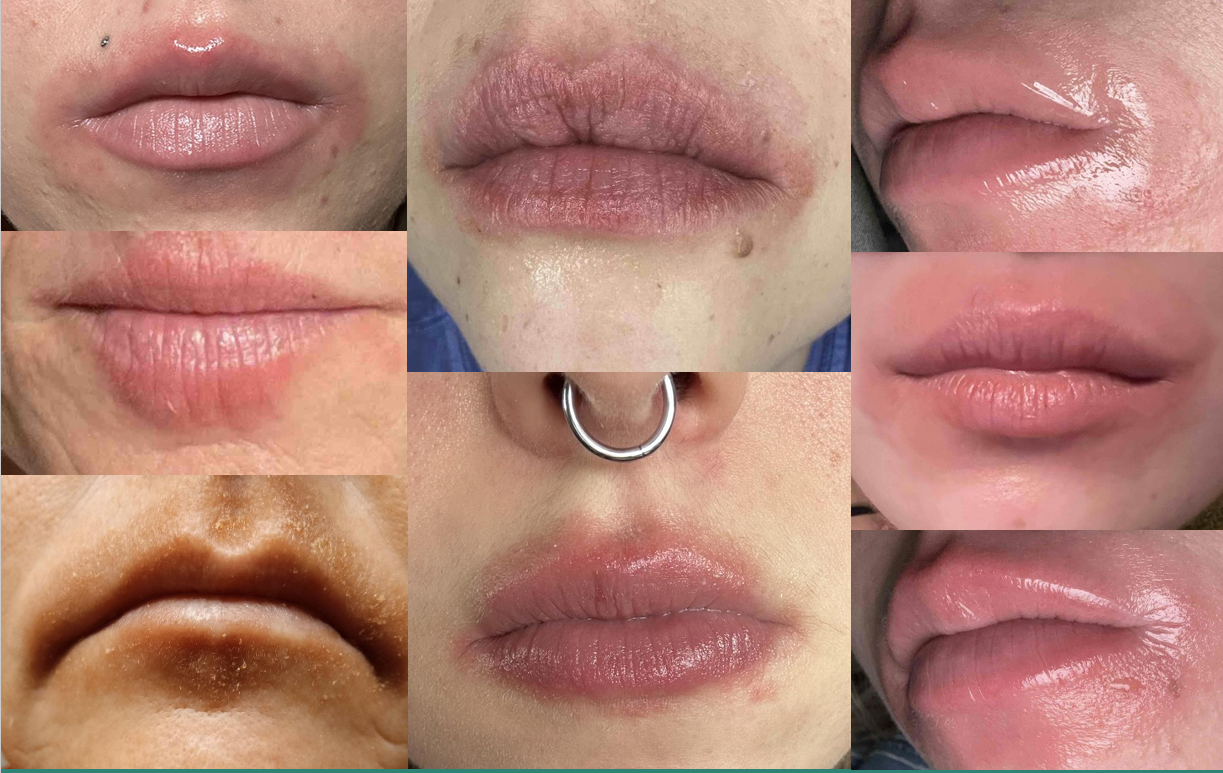

Conclusion: Treating Allergic Contact Dermatitis
Effective treatment of allergic contact dermatitis centers on a stepwise, severity-based approach combined with strict trigger avoidance. In mild cases, restoring the skin barrier with frequent moisturization and switching to gentle, non-irritating cleansers is often sufficient.
As the condition becomes more moderate, adding topical anti-inflammatory treatments and protective measures—such as cotton gloves and minimizing exposure to irritants—helps reduce inflammation and promote healing. In more severe cases, prescription-strength topical steroids or compounded therapies may be necessary to control symptoms.
Across all stages, the most important factor is identifying and avoiding the underlying allergen or irritant, as ongoing exposure will continue to trigger flares. Consistent skin care, barrier repair, and minimizing contact with triggers are key to achieving long-term control and preventing recurrence.
Take the first step toward clearer, healthier skin with advanced, personalized treatment strategies
Locations
700 Tenacity Drive #102 Longmont, Colorado, 80504
2801 Remington Street Suite 2, Fort. Collins, Colorado, 80525
Contact
720-818-0533
Office Hours
Monday-Friday 8:00 AM to 6:00 PM Saturday 10 AM to 2 PM Sunday: By Appoinment only

Aesthetics & Medical Lasers Dermatology
Get a Dermatology consultation and customized skin care solutions
Services
Work Hours
- Monday-Friday 8:00 AM to 6:00 PM Saturday 10 AM to 2 PM Sunday: By Appoinment only
- 720-818-0533
- 700 Tenacity Drive #102 Longmont, Colorado, 80504
- 2801 Remington Street Suite 2, Fort. Collins, Colorado, 80525
- Copyrigt © 2026 Aesthetics & Medical Lasers Dermatology
- Terms of Use
- Privacy Policy
